As things stand, hospital patients in England have no legal right to a second medical opinion. But that could soon change, as a campaign to give patients formal entitlement to an urgent second opinion is gathering momentum and gaining support from key figures, including those in government as well as the NHS England Ombudsman. The proposal, called Martha’s rule, is named after a young girl whose life might have been saved by it.
In 2021, 13-year-old Martha Mills died following an injury she sustained while on holiday with her family. Martha was treated at King’s College Hospital in London, where she developed life-threatening sepsis. The inquest following Martha’s death found it was avoidable, and that she would have survived were it not for tragic failures in the medical care she received. These failures included doctors withholding important information about Martha’s condition from her parents and ignoring their concerns.
The proposal, championed by Martha’s mother, Merope Mills, seeks to improve patient safety in hospitals and prevent avoidable deaths like Martha’s by empowering patients and their families to call for treatment reviews and formal second opinions.
Guidance from the General Medical Council (the regulatory body for doctors in England) mentions that in some circumstances – typically when a patient doesn’t agree with a doctor’s decision or opinion – it may be appropriate for doctors to discuss the option of a second opinion. But though patients have a right to ask for a second opinion, there’s no legal requirement for doctors to provide one.
Martha’s rule would give patients and families the right to seek a rapid review by a separate clinical team – or a second opinion from another specialist doctor based in the same hospital but independent of the team around the patient.
Second opinion
There are several similar systems in place around the world. Many of these were introduced following cases like Martha’s.
For example, in Queensland, Australia, Ryan’s rule (named after Ryan Saunders, who died in 2007) gives patients and families the right to escalate concerns beyond the hospital and request a clinical review of the patient’s case. As of 2022, Ryan’s rule had been deployed 7,300 times since it was introduced in 2013. The process has led to clearer communication about care between patients, their families and doctors.
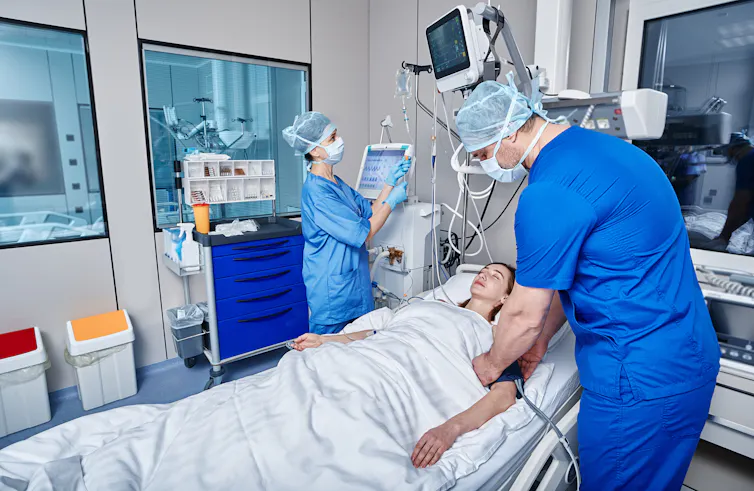
Family-initiated rapid response teams also operate in many US hospitals. When used by a family member, this process provides patients with immediate bedside care from a specialist team. There’s some indication rapid response teams can lead to improved outcomes for patients, including fewer deaths. In one medical centre where this system was introduced, it resulted in markedly fewer cardiac arrests and fewer fatalities from these.
Numerous NHS trusts in England have also introduced “Call 4 Concern” (C4C) – a system which enables patients and families who feel their concerns are not being addressed to escalate the issue to a “critical care outreach team”.
A 2019 review of how the system was operating in the Royal Berkshire Trust (where the model was pioneered) found the service had been used 534 times in seven years – and that 95% of the calls placed were using the service appropriately. In a fifth of cases, significant interventions were required. As the service became established, some staff used it too. There have since been calls to implement the system in all NHS trusts.
It’s clear that such systems can work to improve care for patients. But they are not always straightforward to implement. Some people may lack the confidence to challenge healthcare staff or may not feel they should second-guess a doctor’s opinion, which may inhibit their ability to ask for help. There may be organisational barriers to putting effective systems in place – such as staffing levels and budgetary constraints. There have also been concerns about the potential for inappropriate use or overuse of the facility to request a rapid response (though, as the Royal Berkshire review found, this was minimal).
Over the past decade, there have been considerable changes within the NHS to give greater power and voice to patients and their families. For instance, in 2013 the NHS Constitution was published, which brought patient rights to the fore. In 2015, the landmark case of Montgomery v Lanarkshire Health Board raised the standard that doctors must meet when informing patients about the risks of proposed medical procedures, and about reasonable alternatives.
In 2014, a statutory duty of candour was introduced in England. This includes a legal obligation on health professionals to inform patients and families when something goes wrong, and to apologise.
Advocates for Martha’s rule say it would further “re-balance the power between patients and medics”, and this would undoubtedly be welcome. While the proposal is a necessary step, however, other problems within the NHS – including staff shortages and underfunding – could undermine its impact.
![]()
Mary Neal does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.